Diabetes is a chronic medical condition that affects millions of people worldwide. There are several types of diabetes, but the two most common ones are Type 1 and Type 2 diabetes. While both conditions involve issues with blood sugar regulation, they have distinct differences in terms of causes, symptoms, and management. In this comprehensive blog post, we will delve into the nuances of Type 1 and Type 2 diabetes, helping you better understand these conditions and how to manage them effectively.
What is Diabetes?
Diabetes is a complex metabolic disorder characterized by elevated levels of glucose (sugar) in the blood. This happens when the body cannot effectively regulate the amount of glucose in the bloodstream, leading to high blood sugar levels, which can have serious health consequences.
The Role of Insulin
The hormone insulin plays a crucial role in regulating blood sugar levels. It is produced by the pancreas and helps transport glucose from the blood into cells, where it can be used for energy. When there is an issue with insulin production or utilization, diabetes can develop.
How the Body Regulates Blood Sugar
In a healthy individual, the body constantly monitors blood sugar levels and adjusts insulin production accordingly. This ensures that blood sugar remains within a normal range. However, in diabetes, this finely-tuned system goes awry.
Consult with a General Physician to get a personalized diabetes management plan that suits your specific needs and goals.
Type 1 Diabetes
Causes and Risk Factors
Type 1 diabetes is an autoimmune condition. It occurs when the body's immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. The exact cause of this immune response is still not fully understood, but genetics and environmental factors are believed to play a role.
Symptoms
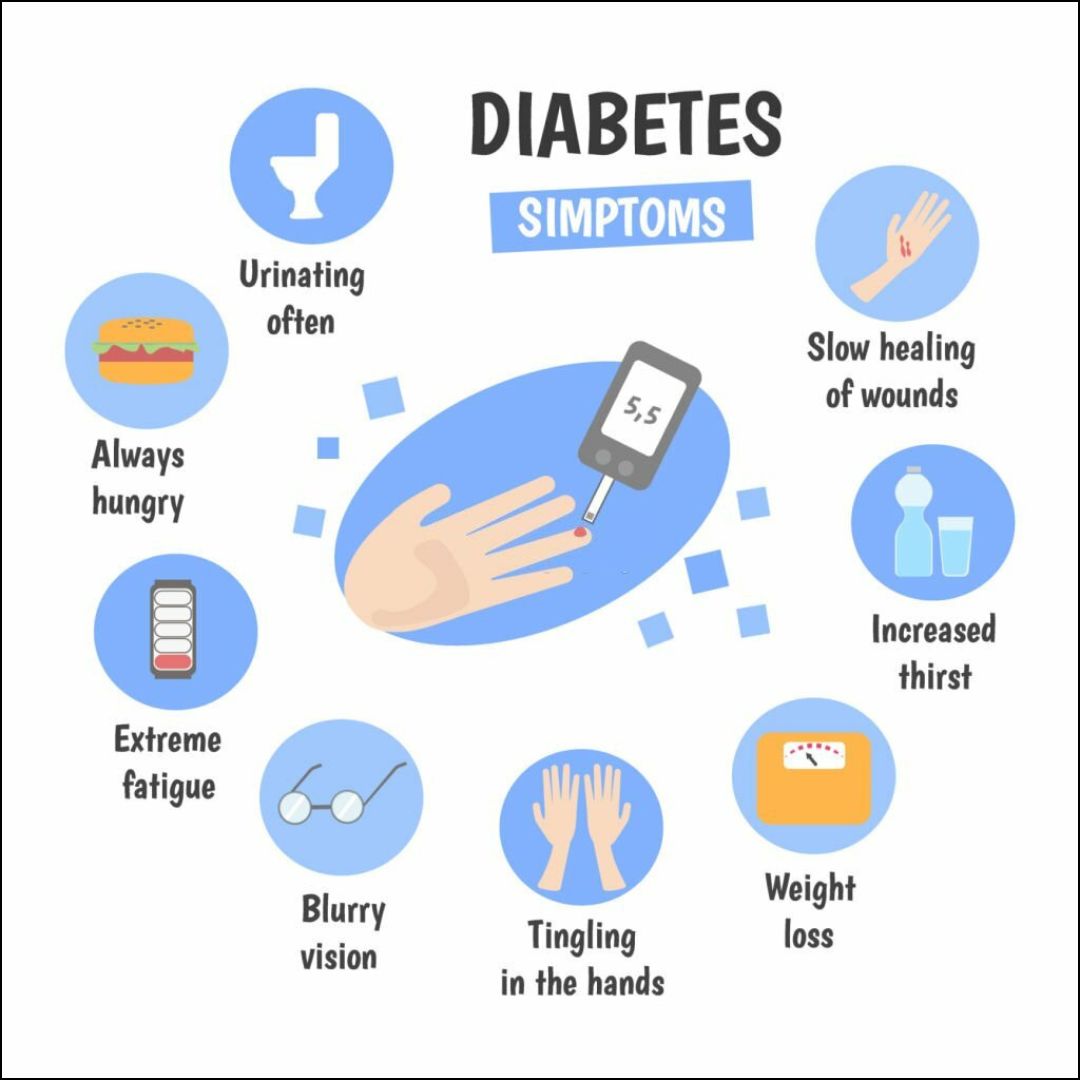
Type 1 diabetes often presents suddenly and severely. Common symptoms include excessive thirst, frequent urination, unexplained weight loss, extreme fatigue, and blurred vision.
Diagnosis
Diagnosis usually involves blood tests to measure blood sugar levels and other markers. Specific tests, like the A1C test, can help determine long-term blood sugar control.
Treatment and Management
People with Type 1 diabetes rely on insulin therapy to replace the hormone their body no longer produces. This can be administered through injections or insulin pumps. Additionally, monitoring blood sugar levels, maintaining a healthy diet, and staying physically active are essential components of management.
Type 2 Diabetes
Causes and Risk Factors
Type 2 diabetes is primarily associated with insulin resistance, where the body's cells do not respond effectively to insulin. Genetic factors, obesity, poor diet, and a sedentary lifestyle are common risk factors for developing Type 2 diabetes.
Symptoms
The onset of Type 2 diabetes is often gradual, and some people may not experience noticeable symptoms initially. However, common symptoms can include increased thirst, frequent urination, fatigue, and slow wound healing.
Diagnosis
Diagnosis typically involves blood tests, including fasting blood sugar levels and oral glucose tolerance tests.
Treatment and Management
Management of Type 2 diabetes includes lifestyle changes such as dietary modifications, regular physical activity, and, in some cases, medication or insulin therapy. Weight loss and blood sugar monitoring are important aspects of control.
Differences Between Type 1 and Type 2 Diabetes
Onset and Age of Diagnosis
Type 1 diabetes often presents in childhood or early adulthood, whereas Type 2 diabetes is more common in adults and is often associated with aging and lifestyle factors.
Autoimmune Response vs. Insulin Resistance
The underlying causes of the two types of diabetes are distinct. Type 1 is an autoimmune disease, while Type 2 is primarily driven by insulin resistance.
Treatment Approaches
Type 1 diabetes requires insulin replacement therapy from the start, while Type 2 diabetes may initially be managed with lifestyle changes and oral medications before progressing to insulin therapy in some cases.
Lifestyle Factors
Lifestyle modifications, including weight management and physical activity, play a more significant role in managing Type 2 diabetes.
Prevention and Risk Reduction
Lifestyle Modifications
Making healthy lifestyle choices, such as maintaining a balanced diet, engaging in regular physical activity, and managing stress, can reduce the risk of developing Type 2 diabetes.
Genetic Factors
Understanding your family history and genetic predispositions can help identify potential risks and take proactive steps toward prevention.
Regular Check-ups
Regular medical check-ups and screenings are crucial for early detection and management of diabetes.
Living with Diabetes
Emotional and Psychological Aspects
The emotional impact of living with diabetes can be significant. Coping strategies and psychological support are crucial for overall well-being.
Dietary Guidelines
Balancing carbohydrate intake, monitoring portion sizes, and paying attention to the glycemic index can help individuals with diabetes manage their blood sugar levels.
Physical Activity
Regular exercise not only helps with blood sugar control but also improves overall health and reduces the risk of complications.
Medications and Insulin
Understanding the different medications and insulin types available is essential for effective diabetes management.
The Importance of Diabetes Awareness
Raising awareness about diabetes is crucial to encourage early diagnosis and effective management.
Empowering People with Diabetes
Ultimately, diabetes is a manageable condition, and with the right information and support, individuals can lead healthy and fulfilling lives despite their diagnosis.
In conclusion, understanding the key differences between Type 1 and Type 2 diabetes is essential for effective management and prevention. By recognizing the risk factors, symptoms, and treatment options for each type, individuals can take control of their health and work towards a better quality of life, whether they are living with diabetes or seeking to prevent it. Diabetes is a global health concern, and raising awareness
Consult with a General Physician to get a personalized diabetes management plan that suits your specific needs and goals.
Related Post Article
1. Managing Blood Sugar Levels: Tips and Tricks for Diabetics
.webp)