Frequently Asked Questions
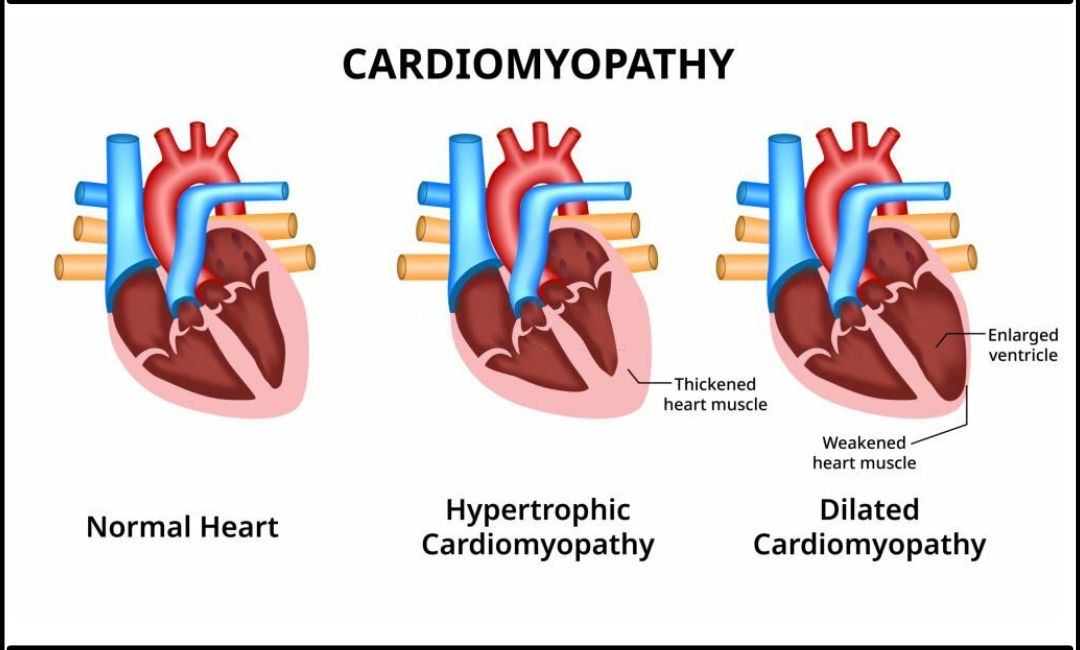
Cardiomyopathy is a serious condition that affects the heart muscle and can have significant implications for one's overall health. This condition is characterized by the weakening or enlargement of the heart muscle, which can lead to symptoms such as shortness of breath, fatigue, and irregular heart rhythms.
Cardiomyopathy can be caused by a variety of factors, including genetics, infections, certain medications, and underlying medical conditions. It is important for individuals with cardiomyopathy to receive proper medical care and management to prevent further complications and improve their quality of life.
One of the primary risk factors for developing cardiomyopathy is a family history of the disease. If you have a close relative, such as a parent or sibling, who has been diagnosed with cardiomyopathy, it increases your chances of developing it as well.
Common symptom of cardiomyopathy is shortness of breath, which may occur during physical activity or even at rest. This can be a result of the heart's inability to pump blood effectively due to weakened or stiffened muscles. Fatigue and weakness are also frequently experienced by individuals with cardiomyopathy, as the heart struggles to meet the body's demands for oxygen-rich blood.
Accurate and timely diagnosis of cardiomyopathy is crucial for effective management and treatment of this cardiac condition. With advancements in medical technology, healthcare professionals now have access to a range of diagnostic tools and techniques that aid in the identification and classification of cardiomyopathy.
One common aspect of cardiomyopathy treatment is lifestyle modifications. This can include adopting a heart-healthy diet, engaging in regular exercise (under medical supervision), quitting smoking, and managing stress levels. These lifestyle changes can help improve overall heart health and potentially slow down the progression of cardiomyopathy. For some individuals with more severe forms of cardiomyopathy or those who do not respond well to medication therapy alone, advanced treatments may be considered. These can include implantable devices such as pacemakers or implantable cardioverter-defibrillators (ICDs) to help regulate heart rhythm or assist with pumping blood effectively.
One of the most crucial aspects of preventing cardiomyopathy is adopting a healthy lifestyle. This includes maintaining a balanced diet that is low in saturated fats, cholesterol, and sodium while being rich in fruits, vegetables, whole grains, and lean proteins. Regular physical activity is also essential in preventing cardiomyopathy as it helps to maintain a healthy weight, lower blood pressure, and improve cardiovascular fitness.
.webp)


 040 6700 0000
040 6700 0000  040 6700 0111
040 6700 0111