Frequently Asked Questions
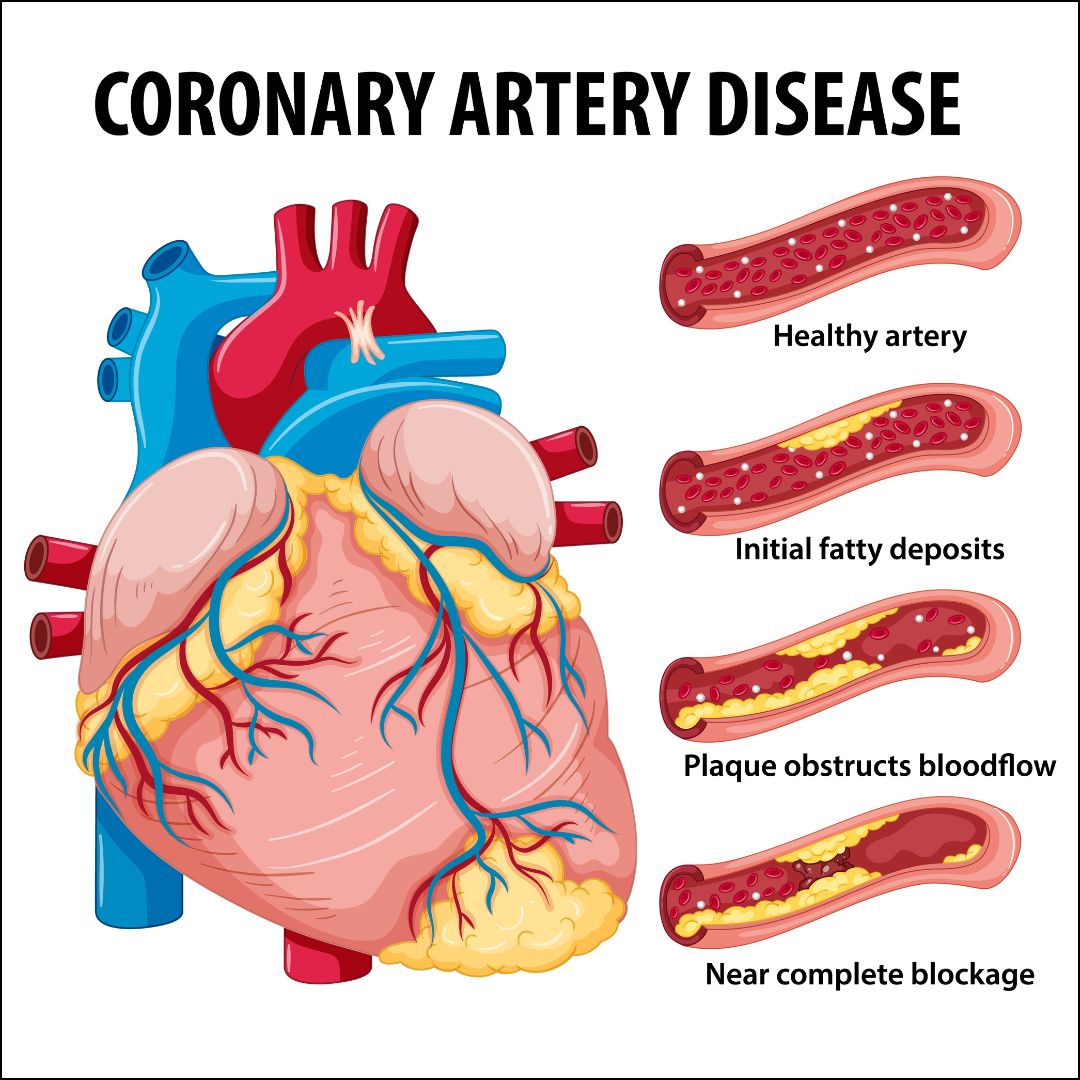
Coronary Artery Disease (CAD) is a prevalent and serious medical condition that affects millions of people worldwide. It refers to the narrowing or blockage of the coronary arteries, which supply oxygen-rich blood to the heart muscle. CAD is primarily caused by a buildup of plaque inside the arteries, a condition known as atherosclerosis.
Coronary artery disease is primarily caused by a buildup of plaque inside the arteries, a condition known as atherosclerosis. This plaque is made up of cholesterol, fat, calcium, and other substances that accumulate over time. As the plaque continues to grow, it restricts blood flow to the heart, leading to various symptoms such as chest pain (angina), shortness of breath, fatigue, and in severe cases, heart attacks.
Understanding coronary artery disease and its risk factors is crucial for early detection and prevention. Age, family history of heart disease, high blood pressure (hypertension), high cholesterol levels (hyperlipidemia), smoking, diabetes mellitus, obesity, sedentary lifestyle, and stress are some common risk factors associated with coronary artery disease.
One common symptom of coronary artery disease is chest pain or angina. This pain may feel like pressure, tightness, or a squeezing sensation in the chest. It can also radiate to the arms, shoulders, neck, jaw, or back. Shortness of breath is another symptom that individuals with coronary artery disease may experience. This can occur during physical activity or even at rest. Fatigue and weakness are also commonly reported symptoms, as the heart muscle may not be receiving enough oxygen-rich blood.
One of the primary diagnostic tools used for coronary artery disease is the coronary angiography. This invasive procedure involves the insertion of a catheter into the blood vessels to visualize any blockages or narrowing in the coronary arteries. It provides detailed images that help determine the extent and severity of coronary artery disease. Another non-invasive method commonly employed is stress testing. This involves monitoring the heart's response to physical exertion or medication-induced stress while measuring various parameters such as heart rate, blood pressure, and electrocardiogram (ECG).
One of the primary goals in treating coronary artery disease is to reduce the risk of complications and improve overall heart health. Lifestyle modifications play a crucial role in this regard. This can include adopting a heart-healthy diet, engaging in regular exercise, quitting smoking, and managing stress levels. In addition to lifestyle changes, medication therapy is often prescribed to manage coronary artery disease. Medications such as antiplatelet drugs, beta-blockers, statins, and angiotensin-converting enzyme (ACE) inhibitors may be used to control symptoms, lower blood pressure and cholesterol levels, prevent blood clots, and reduce the workload on the heart.
One of the most effective ways to prevent coronary artery disease is through maintaining a balanced diet. Consuming a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats can help control cholesterol levels and blood pressure. Limiting the intake of saturated fats, trans fats, sodium, and added sugars is also crucial in promoting heart health. Regular physical activity plays a vital role in preventing coronary artery disease as well.
.webp)


 040 6700 0000
040 6700 0000  040 6700 0111
040 6700 0111