Frequently Asked Questions
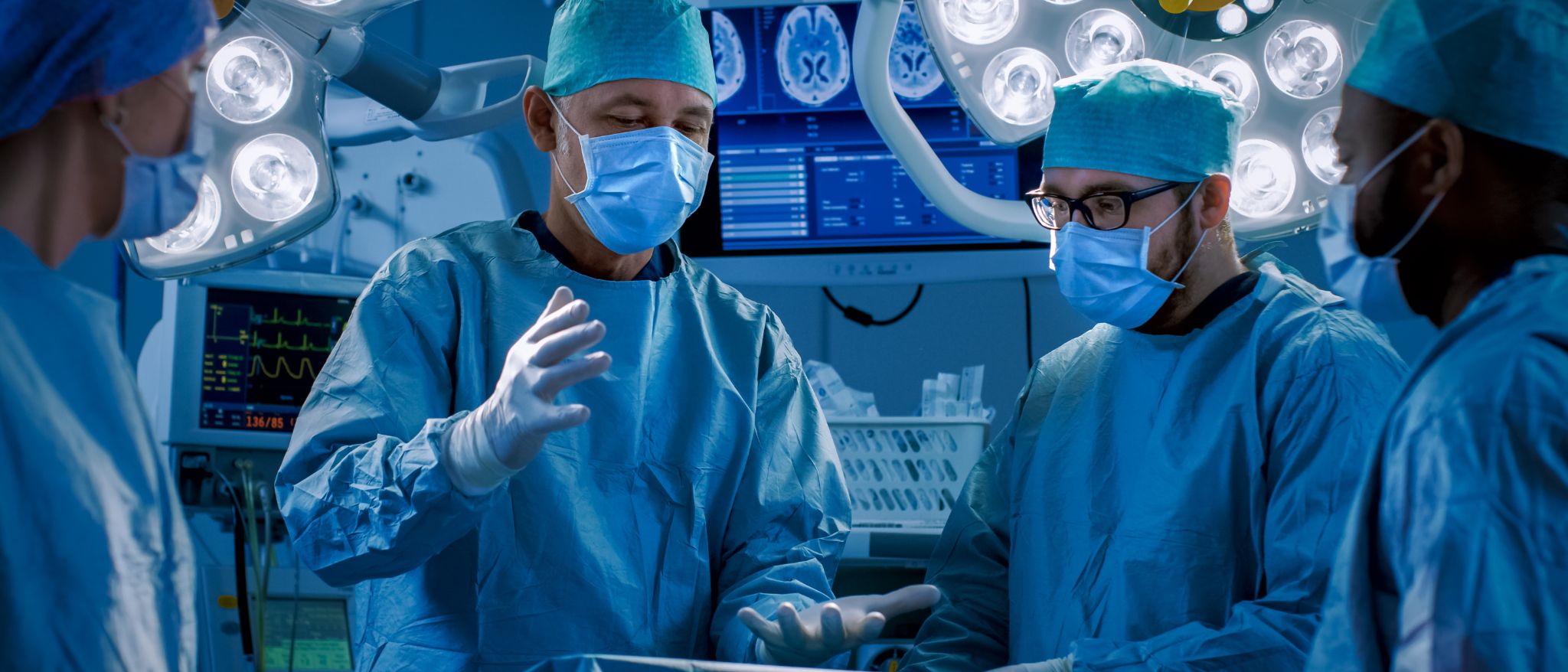
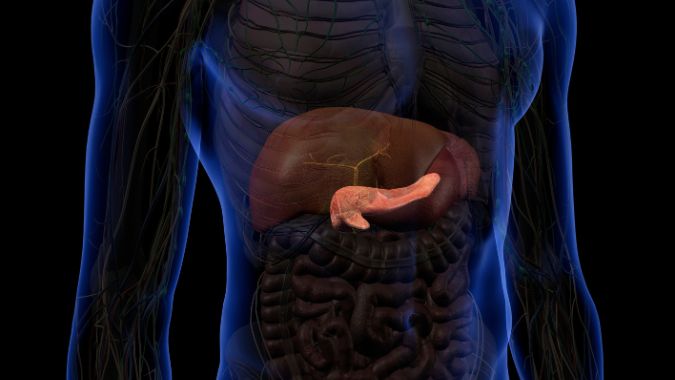
A pancreas transplantation is a surgical procedure where a healthy pancreas is transplanted into a person whose pancreas is not functioning properly. It's usually done for individuals with type 1 diabetes whose blood sugar levels are difficult to control.
The transplant surgery involves removing the diseased pancreas and replacing it with a healthy pancreas from a deceased donor. The new pancreas is connected to blood vessels and the digestive system.
Risks include those associated with any major surgery, such as infection, bleeding, and complications related to anesthesia. Additionally, there is a risk of rejection, where the recipient's immune system attacks the transplanted pancreas.
The success rate of pancreas transplantation varies depending on factors such as the recipient's overall health and the quality of the donor pancreas. Generally, success rates have improved over time with advancements in surgical techniques and immunosuppressive medications.
Recovery after a pancreas transplant involves staying in the hospital for a period of time for monitoring and management of any complications. Patients will need to take immunosuppressive medications for the rest of their lives to prevent rejection and will require close follow-up care with their transplant team.
Many pancreas transplant recipients experience improved quality of life and better blood sugar control following transplantation. However, long-term outcomes can vary, and some recipients may experience complications or require additional medical interventions over time.
.webp)


 040 6700 0000
040 6700 0000  040 6700 0111
040 6700 0111